Quick Answer: What is the difference between ERA and EOB?
ERA (Electronic Remittance Advice) is an electronic document sent to healthcare providers that explains how an insurance claim was paid, adjusted, or denied and drives automated payment posting in billing software. EOB (Explanation of Benefits) is a document sent to patients describing how their insurance processed the same claim. An EOB is not a bill, it is an informational summary of an insurancebenefit application.
If you work in healthcare billing or you are a patient trying to understand a document from your insurance company, you have almost certainly encountered the terms ERA and EOB. Both documents are generated after an insurance claim is adjudicated. Still, they serve completely different purposes and reach completely different audiences.
This guide covers everything: definitions, key differences, real-world examples, how to read each document, common billing codes, and where ERA and EOB fit into the medical billing process.
Table of Contents
What Is ERA in Medical Billing?
Definition:
Electronic Remittance Advice (ERA) is a digital document sent by an insurance payer to a healthcare provider after a claim is adjudicated. It details how much was paid, what was adjusted, and the reason for any denials. It is used for automated payment posting in medical billing software.
ERA is transmitted through Electronic Data Interchange (EDI) using the HIPAA-compliant ANSI X12 835 transaction standard. This structured format allows billing software to automatically import, match, and post ERA data, eliminating manual data entry and reducing payment errors.
ERA files are commonly received through a medical billing clearinghouse, which connects insurance payer systems with the provider’s revenue cycle management (RCM) software. This connection makes automated payment posting possible.
ERA Entity Attributes
Key attributes of the ERA document:
| ERA Attribute | Detail |
| File Format | ANSI X12 835 electronic transaction |
| Transmission Standard | HIPAA Electronic Data Interchange (EDI) |
| Delivery Method | Insurance payer → clearinghouse → billing software |
| Automation | Automatically imported and posted by billing software |
| Contains | Payments, contractual adjustments, CARC codes, denials |
| Recipient | Healthcare provider / billing team |
| Processing Speed | Usually within 1–5 business days |
| Governing Body | Centers for Medicare & Medicaid Services (CMS) |
ERA helps billing teams:
- Post payments automatically without manual data entry
- Identify claim adjustments and contractual write-offs
- Reconcile insurance reimbursements against billed amounts
- Reduce manual billing work and human error
- Flag denied claims for follow-up in the denial management workflow
What Is EOB in Medical Billing?
Definition:
Explanation of Benefits (EOB) is a document sent by an insurance company to the patient after a medical claim is processed. It explains how the insurer handled the claim, what was paid to the provider, and what, if anything, the patient may owe. An EOB is not a bill.
The EOB is written in plain language for patients, not billing professionals. It translates the technical payment decision into a readable summary showing the patient their deductible, copay, and coinsurance breakdown.
EOB Entity Attributes
| EOB Attribute | Detail |
| Document Type | Paper letter, PDF, or online portal document |
| Sent By | Insurance payer directly to the patient |
| Purpose | Patient explanation of insurance benefit application |
| Coverage Breakdown | Shows deductible, copay, coinsurance, and plan payment |
| Appeal Instructions | Includes how to dispute or appeal the claim decision |
| Recipient | Patient / insurance policyholder |
| Timing | 1–3 weeks by mail; faster via online portal |
| Is It a Bill? | No, it is an informational summary, not a payment request |
ERA vs EOB: Key Differences
Here is a side-by-side comparison across every important dimension:
| Feature | ERA (Electronic Remittance Advice) | EOB (Explanation of Benefits) |
| Sent To | Healthcare provider / billing team | Patient / insurance policyholder |
| Format | Electronic file – ANSI X12 835 | Paper letter, PDF, or online portal |
| Purpose | Automated payment posting & reconciliation | Inform patient of claim results and costs |
| Delivery | Clearinghouse → billing software | Mail or patient online portal |
| Processing | Automated, imported into billing software | Manual review by patient |
| Contains Denial Codes | Yes – CARC & GRC codes (technical) | Yes – simplified, patient-friendly language |
| HIPAA Standard | Yes – HIPAA 835 transaction | Not a mandated HIPAA transaction |
| Speed | 1–5 business days | 1–3 weeks by mail |
| Is It a Bill? | No, payment explanation | No, informational summary |
| Action Required | Post payment; follow up on denials | Review; wait for provider statement |
Key takeaway: ERA and EOB carry the same underlying claim data, but ERA is a machine-readable tool for billing teams, while EOB is a plain-language summary for patients.
ERA vs EOB Example
The fastest way to understand ERA and EOB is to see them side by side on the same real claim:
The Scenario
- Patient visits a family medicine clinic for an office visit and a blood panel.
- Provider bills $320 to the patient’s commercial insurance.
- Insurance adjudicates the claim based on the contracted fee schedule and the patient’s deductible status.
- Payer sends an ERA to the provider’s billing team and an EOB to the patient.
Same Claim – Two Documents
| Claim Detail | ERA – What the Billing Team Sees | EOB – What the Patient Sees |
| Service | Office visit + blood panel | Office visit + blood panel |
| Billed Amount | $320.00 | $320.00 |
| Allowed Amount | $210.00 | $210.00 |
| Plan Discount / Adjustment | –$110.00 (CARC: CO-45) | –$110.00 (shown as plan discount) |
| Deductible Applied | $100.00 (CARC: PR-1) | $100.00 (applied to your deductible) |
| Insurance Payment | $110.00 | $110.00 |
| Patient Responsibility | $100.00 | $100.00 (what you may owe) |
| Document Format | ANSI X12 835 electronic file | Paper letter or PDF |
| Required Action | Post $110 payment; bill patient $100 | Review and wait for provider statement |
In this example, CARC CO-45 tells the billing team to write off $110 as a contractual obligation. PR-1 confirms $100 is the patient’s deductible, not a denial. The billing software posts all of this automatically from the ERA 835 file.
The patient’s EOB tells the same story in plain language: $110 in plan discounts, $110 paid by insurance, and $100 owed toward their deductible. The patient should wait for the provider’s statement before paying.
Where ERA and EOB Fit in the Medical Billing Process
ERA and EOB are generated at the same point in the medical billing process, immediately after the insurer completes claim adjudication. Here is the complete workflow:
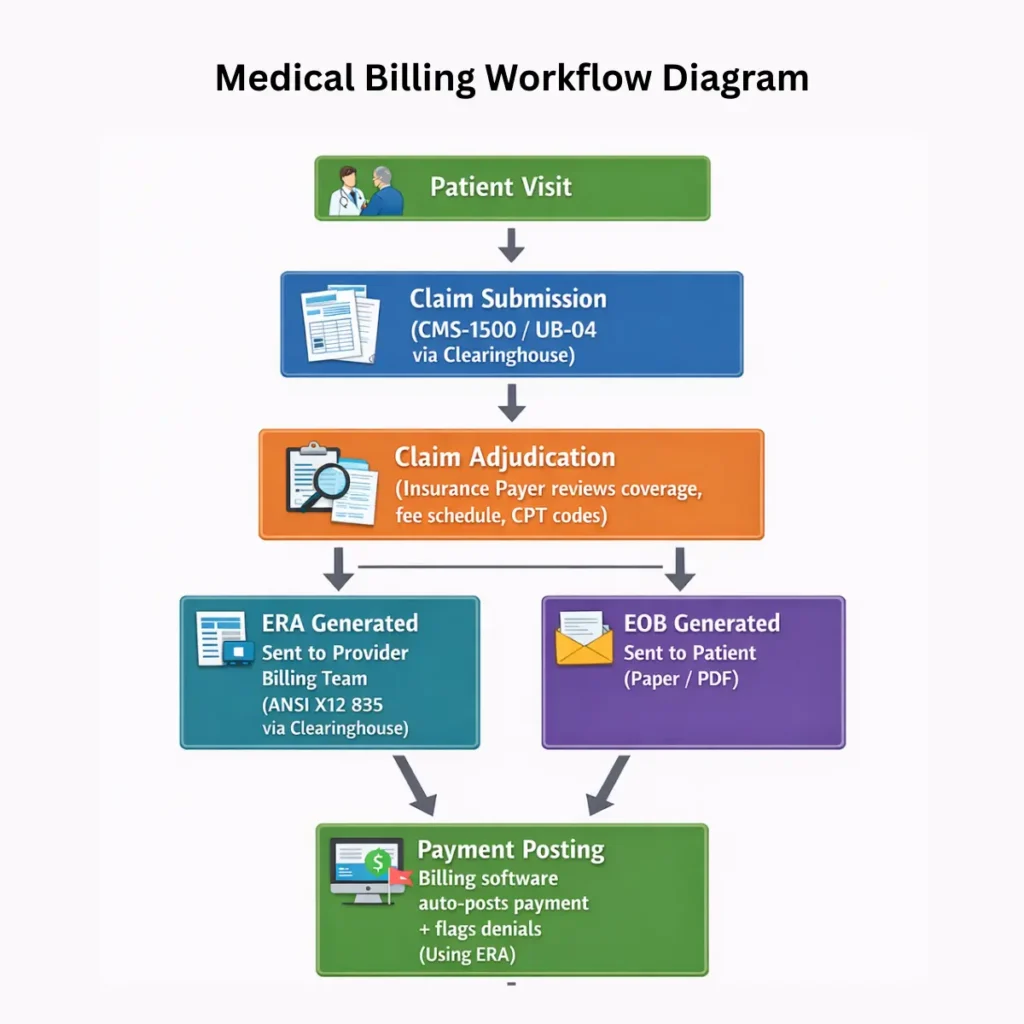
The diagram above shows how ERA and EOB split at the adjudication stage. ERA goes left to the billing team for payment posting; EOB goes right to the patient for their records. Here is the same workflow in table form:
| Step | Stage | What Happens |
| 1 | Patient Visit | Patient receives medical services from a healthcare provider. |
| 2 | Claim Submission | Provider submits claim (CMS-1500 or UB-04) to the insurance payer through a clearinghouse using EDI standards. |
| 3 | Claim Adjudication | The insurance payer reviews the claim, evaluating coverage, medical necessity, CPT codes, and contracted fee schedule. |
| 4 | ERA Generated | ERA is sent electronically to the provider’s billing team as an ANSI X12 835 transaction via clearinghouse. |
| 5 | EOB Generated | EOB is mailed or emailed to the patient summarizing the insurer’s payment decision in plain language. |
| 6 | Payment Posting | Billing team imports the ERA into the billing software for automated payment posting and AR reconciliation. Any claim not fully resolved at this stage enters the AR aging workflow, tracked and managed through a structured AR aging report that drives follow-up across every unpaid bucket. |
How to Read an ERA
Reading an ERA correctly is essential for accurate payment posting. Here is what billing teams should check on every ERA:
- Match the claim number: Verify the ERA claim reference matches the original claim in your billing system before posting anything.
- Check the NPI and payer ID: Confirm the ERA is addressed to the correct provider and from the correct payer.
- Review billed vs. allowed amount: The difference is the contractual adjustment (CO-45). Verify this matches your contracted fee schedule.
- Read every CARC code: Each adjustment or denial has a reason code. Never skip these; they explain exactly what happened to the payment.
- Identify patient responsibility: Note deductible (PR-1), coinsurance (PR-2), and copay (PR-3) amounts before generating patient statements.
- Flag zero-payment lines: A $0 payment is not always a denial. CO-97 means the service was bundled into another paid procedure. Read the code first.
- Check the EFT or check reference: Match the ERA payment to the bank deposit to confirm the funds arrived correctly.
Accurate ERA reading directly determines the accuracy of every patient statement your practice generates. Errors at this stage cascade into billing disputes, overpayments, and collections problems.
How to Read an EOB
Most patients find EOBs confusing. Here is a simple step-by-step guide:
- If something looks wrong, use the appeal instructions: Every EOB includes a process for disputing the insurer’s decision. Act within the stated deadline.
- Find ‘Patient Responsibility’ or ‘Amount You Owe’: This is the most important number. It shows what the provider may bill you.
- Check service dates and descriptions: Confirm dates and procedures match the care you actually received. Errors here could indicate billing mistakes or fraud.
- Look at ‘Plan Paid’: What your insurance paid the provider. If you expected full coverage and this is $0, check the next column for the reason.
- Review the ‘Not Covered’ column: Services here are excluded from your plan. If you believe something should be covered, this is the basis for an appeal.
- Note the deductible applied: If your deductible has not been met, more of the cost shifts to you. Track this against your annual deductible total.
- Do not pay based on the EOB: Wait for the provider’s official statement, which should match the EOB’s patient responsibility amount.
Remember: The EOB is from your insurer. The bill is from your provider. Always compare the two before paying.
Common Codes in ERA and EOB
CARC Codes (Claim Adjustment Reason Codes) Found in ERA
CARC codes appear on every ERA and explain every payment adjustment. Billing teams must understand these to post payments correctly and manage denials effectively.
| CARC Code | Group Code | What It Means for Billing |
| CO-45 | CO (Contractual Obligation) | Charges exceed contracted fee schedule, standard write-off |
| PR-1 | PR (Patient Responsibility) | Amount applied to patient’s annual deductible |
| PR-2 | PR (Patient Responsibility) | Amount applied to patient’s coinsurance |
| PR-3 | PR (Patient Responsibility) | Amount applied to patient’s copay |
| CO-97 | CO (Contractual Obligation) | Service bundled into another paid procedure, not a denial |
| CO-4 | CO (Contractual Obligation) | Service inconsistent with modifier submitted |
| CO-96 | CO (Contractual Obligation) | Non-covered service, not in patient’s benefit plan |
| OA-23 | OA (Other Adjustment) | Adjusted due to prior payer adjudication (coordination of benefits) |
| CO-50 | CO (Contractual Obligation) | Non-covered, not deemed medically necessar |
Common Terms Found in EOB
| EOB Term | What It Means in Plain Language |
| Billed Charge | Total amount the provider charged for the service |
| Plan Discount | The contractual adjustment, same as CO-45 on the ERA |
| Plan Paid | Amount the insurer paid directly to the provider |
| Deductible | Amount applied toward your annual out-of-pocket deductible |
| Copay | Fixed dollar amount you pay at time of service |
| Coinsurance | Your percentage share of covered costs after deductible is met |
| Amount You Owe | Total patient responsibility, what you may owe your provider |
| Not Covered | Service excluded from your insurance plan benefits |
| Claim Number | Reference number for calling to dispute or appeal |
Why Do Patients Receive an EOB?
Direct Answer:
Patients receive an EOB because insurance companies are required to notify policyholders of how their claims were processed. The EOB is the insurer’s official communication to the patient explaining coverage applied, amounts paid, and any remaining patient responsibility. It is not a bill.
- Transparency requirement: Regulations require insurers to inform policyholders how their benefits were applied to every claim.
- Cost awareness: The EOB helps patients understand out-of-pocket costs before they receive a provider bill so that they can budget accordingly.
- Fraud detection: EOBs allow patients to verify that the services listed were actually received. A service the patient did not receive could be a billing error or insurance fraud.
- Appeal rights: Every EOB includes instructions for how to dispute the insurer’s decision if the patient believes the claim was incorrectly processed.
- Coordination of benefits: For patients with multiple insurance plans, the EOB shows how the primary insurer processed the claim information needed by the secondary insurer.
Why an EOB Is Not a Medical Bill
This is one of the most common points of confusion in healthcare. Here is the key distinction:
| EOB (Explanation of Benefits) | Medical Bill / Provider Statement |
| Sent by the insurance company | Sent by the healthcare provider |
| Arrives before or alongside the provider bill | Arrives after the ERA is posted by billing team |
| Shows how insurance processed the claim | Shows the balance actually owed to the provider |
| Does not request payment | Requests payment from the patient |
| From insurer to patient | From provider to patient |
| Informational notice | Official billing statement |
Important: If you receive an EOB but no bill from your provider yet, do not pay. If the provider’s bill does not match your EOB, contact the provider’s billing office first, then your insurer.
Is ERA the Same as EOB?
Direct Answer:
No. ERA and EOB are not the same document. Both are generated from the same insurance claim adjudication, but they serve different purposes and go to different recipients. ERA is sent to the healthcare provider’s billing team for payment posting. EOB is sent to the patient to explain how their insurance was applied.
- ERA is machine-readable: An ANSI X12 835 file imported by billing software, not read by humans directly.
- EOB is human-readable: A formatted letter or PDF in plain language for a patient with no billing background.
- ERA is the billing team’s tool for payment posting, denial management, and revenue cycle reconciliation.
- EOB is the patient’s tool for understanding costs, verifying claim accuracy, and exercising appeal rights.
Think of it this way: ERA is the back-office payment record that the accounting team processes. EOB is the customer-facing summary that explains the same transaction to the patient.
ERA vs EOB vs RA: Understanding All Three Documents
In medical billing, three related documents often confuse: ERA, EOB, and RA (Remittance Advice). Here is how they differ:
| Feature | ERA | EOB | RA (Remittance Advice) |
| Full Name | Electronic Remittance Advice | Explanation of Benefits | Remittance Advice |
| Format | Electronic, ANSI X12 835 | Paper / PDF | Paper check stub or letter |
| Sent To | Provider billing team | Patient | Provider billing team |
| Purpose | Automated payment posting | Patient claim explanation | Manual payment reconciliation |
| Processing | Automated by billing software | Manual review by patient | Manual data entry required |
| Still Used? | Yes, primary standard | Yes, always issued | Being phased out; ERA preferred |
The key difference between ERA and RA is format. RA is the older paper version of the same payment explanation. ERA replaced it with an electronic 835 file that billing software processes automatically. Most modern payers use ERA; paper RA is now largely phased out.
Benefits of ERA for Healthcare Providers
ERA is one of the most impactful efficiency tools in modern medical billing:
- Automated payment posting: ERA files import directly into billing software, posting hundreds of payments in minutes instead of hours of manual entry.
- Faster cash flow: Electronic delivery means ERA files arrive in 1–5 business days. Paper RA can take weeks, delaying reimbursements.
- Reduced billing errors: Automated posting eliminates transcription errors from manual data entry.
- Better denial management: Standardized CARC codes make it easy to sort and prioritize denied claims for appeals. Once CARC codes identify a denied claim, the AR follow-up process begins. See how billing teams resolve each denial type in our guide to AR follow-up in medical billing.
- HIPAA compliance: Using ANSI X12 835 transactions through EDI satisfies federal electronic data interchange requirements.
- Improved payment reconciliation: ERA data verifies every claim is paid at the correct contracted rate, catching underpayments before they age.
- Audit-ready records: ERA files provide a complete, timestamped electronic record of every payer payment decision.
For more, see our Healthcare EDI Guide and our overview of Revenue Cycle Management services.
Common Questions About ERA vs EOB
Here are quick answers to the questions billing teams and patients ask most often:
Is ERA the same as Remittance Advice (RA)?
Yes and no. ERA and RA contain the same payment information, but ERA is the electronic version (ANSI X12 835) while RA is the older paper version attached to a check. ERA is now the industry standard because billing software can process it automatically. Paper RA still exists but is largely being phased out.
Can patients receive an ERA?
No. ERA is sent only to the healthcare provider’s billing team via a clearinghouse. Patients receive an EOB instead. However, a patient can request a copy of their ERA from their provider if they are disputing a billing claim or trying to verify how their claim was posted.
Do providers see the EOB?
Not typically. The EOB is sent by the insurer directly to the patient. However, providers can request a copy of a patient’s EOB and often do when a patient disputes their bill or when the ERA and patient-reported information don’t match.
Why does the EOB arrive before the provider’s bill?
The EOB is generated by the insurance company and mailed immediately after claim adjudication. The provider’s bill only comes after the billing team receives and posts the ERA, which may take a few additional days. This timing gap is why patients should never pay based on the EOB alone.
What happens if the ERA and EOB amounts don’t match?
If the ERA shows a different payment amount than the EOB, it is likely a timing difference, a coordination of benefits issue, or a payer error. The billing team should contact the payer to investigate and request a corrected ERA or EOB if necessary. Do not post ERA payments that do not reconcile with the EOB without investigation.
Frequently Asked Questions About ERA and EOB
What does ERA stand for in medical billing?
ERA stands for Electronic Remittance Advice. It is a digital document sent by insurance payers to healthcare providers after a claim is processed, detailing payments, adjustments, and denials. Used for automated payment posting in revenue cycle management software.
What does EOB mean in healthcare?
EOB stands for Explanation of Benefits. It is a document sent by the insurance company to the patient after a claim is processed, explaining how the claim was handled and what the patient may owe. An EOB is not a bill, it is an informational summary of how insurance benefits were applied.
What is the difference between ERA and EOB?
ERA is sent to the provider’s billing team for automated payment posting. EOB is sent to the patient to explain how their insurance was applied. Both carry the same claim data: ERA is machine-readable for billing systems, EOB is plain-language for patients.
Is ERA the same as EOB?
No. ERA goes to the provider’s billing team in ANSI X12 835 electronic format for automated payment posting. EOB goes to the patient in plain language (paper or PDF) to explain the insurer’s payment decision. They contain similar data but serve different audiences entirely.
Is an EOB the same as a bill?
No. An EOB is not a medical bill. It is an informational notice from the insurance company. Patients should always wait for an official provider statement before making payments. Paying based on the EOB alone can result in overpayment or paying the wrong party.
Why do patients receive an EOB?
Patients receive an EOB because insurers are required to notify policyholders of how their claims were processed. The EOB promotes transparency, helps patients understand out-of-pocket costs, enables fraud detection, and provides the information needed to appeal a claim decision.
What is ERA 835 in medical billing?
ERA 835 refers to the ANSI X12 835 Health Care Claim Payment/Advice transaction, the HIPAA-mandated electronic format all US insurance payers use to send payment and remittance information to healthcare providers. All modern billing software can automatically import and post 835 ERA files.
How long does it take to receive ERA after claim submission?
Most ERA files arrive within 1 to 5 business days after the insurance company adjudicates the claim. The timeline varies by payer and clearinghouse. Medicare ERA files are typically received within 14 days of claim submission.
What is ERA vs RA in medical billing?
ERA (Electronic Remittance Advice) and RA (Remittance Advice) contain the same payment information in different formats. ERA is an electronic ANSI X12 835 file processed automatically by billing software. RA is the older paper version requiring manual data entry. ERA is now the industry standard; paper RA is largely phased out.
Final Thoughts
ERA and EOB are two sides of the same insurance payment event, one built for billing teams, one built for patients. When both are processed correctly and in sync, the entire revenue cycle runs more smoothly.
- If you run a practice, invest in billing software that processes ERA automatically and consider partnering with an RCM team to handle the full cycle.
- If you are a billing professional: master CARC codes, automate ERA posting, and reconcile every ERA against your fee schedule to catch underpayments.
- If you are a patient, read your EOB carefully, compare it to your provider’s statement, and never pay until you receive an official bill.
Need Help Managing ERA Posting or Revenue Cycle Payments?
Understanding the difference between ERA and EOB is important, but managing ERA files, payment posting, and denial follow-ups can quickly become time-consuming for in-house billing teams.
At MediBill RCM LLC, we help healthcare practices streamline the entire revenue cycle, including ERA processing, payment reconciliation, and denial management.
Our billing specialists can help your practice:
- Automate ERA payment posting and reduce manual work
- Identify underpayments and contractual adjustments
- Resolve denials and claim discrepancies faster
- Improve cash flow and accounts receivable performance
- Ensure HIPAA-compliant billing workflows
If your team is spending too much time managing remittance files or reconciling insurance payments, our experts can help.
Speak with a MediBill RCM specialist today to learn how we can simplify your billing workflow and improve your revenue cycle performance.